|
 If
a traveller indulges in casual sex,
the risk of infection with a sexually transmitted disease
is high. If
a traveller indulges in casual sex,
the risk of infection with a sexually transmitted disease
is high.
Gonorrhoea and syphilis may cause serious long-term
disability, especially if treatment is delayed. Chlamydia
is widespread throughout many countries including European
countries and the UK and is often symptomless and goes unnoticed
for some time. If untreated it can result in sterility. Hepatitis
B and HIV are both also spread sexually and there is currently
no cure for either infection.
 Travellers
should be aware that a person infected with an STD, HIV
or Hepatitis B may appear perfectly healthy and may not even
know that they are infected. Travellers
should be aware that a person infected with an STD, HIV
or Hepatitis B may appear perfectly healthy and may not even
know that they are infected.
Casual sexual intercourse is risky. Unprotected sexual
intercourse should avoided with anyone other than a regular
partner. Always use good quality condoms and carry them rather
than try to obtain them at the last minute. Remember, condoms
provide good but not complete protection.
Alcohol weakens inhibitions and makes it easier to forget
about taking precautions.
Any person who on return from travel has any reason
to believe that they may have picked up an infection should
get a thorough check up at their local VD clinic.
Whilst all STIs are potentially dangerous, the three most
common (Chlamydia, Gonorrhoea & Syphilis) are dealt with
in more depth here:
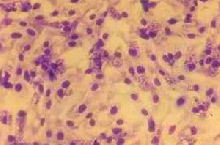 Chlamydia Chlamydia
Chlamydia is a common sexually transmitted disease caused
by the bacterium, Chlamydia trachomatis, which can damage
a woman's reproductive organs. Even though symptoms of chlamydia
are usually mild or absent, serious complications that cause
irreversible damage, including infertility, can occur "silently"
before a woman ever recognizes a problem. Chlamydia also can
cause discharge from the penis of an infected man.
Chlamydia is the currently most frequently reported bacterial
sexually transmitted disease in Western Countries. Under-reporting
is substantial because most people with chlamydia are not
aware of their infections and do not seek testing.
Chlamydia can be transmitted during vaginal, anal, or oral
sex. Chlamydia can also be passed from an infected mother
to her baby during vaginal childbirth.
 Any
sexually active person can be infected with chlamydia. The
greater the number of sex partners, the greater the risk of
infection. Because the cervix (opening to the uterus) of teenage
girls and young women is not fully matured and is probably
more susceptible to infection, they are at particularly high
risk for infection if sexually active. Any
sexually active person can be infected with chlamydia. The
greater the number of sex partners, the greater the risk of
infection. Because the cervix (opening to the uterus) of teenage
girls and young women is not fully matured and is probably
more susceptible to infection, they are at particularly high
risk for infection if sexually active.
Since chlamydia can be transmitted by oral or anal sex, men
who have homosexual sex with other men are also at risk for
chlamydial infection.
Chlamydia is known as a "silent" disease because
the majority of infected people have no symptoms. If symptoms
do occur, they usually appear within 1 to 3 weeks after exposure.
Women who have symptoms might have an abnormal vaginal discharge
or a burning sensation when urinating. If the infection spreads
from the cervix to the fallopian tubes they may develop lower
abdominal pain, low back pain, nausea, fever, pain during
intercourse, or bleeding between menstrual periods. Chlamydial
infection of the cervix can spread to the rectum.
 Men
with signs or symptoms might have a discharge from their penis
or a burning sensation when urinating. Men might also have
burning and itching around the opening of the penis. Pain
and swelling in the testicles are uncommon. Men
with signs or symptoms might have a discharge from their penis
or a burning sensation when urinating. Men might also have
burning and itching around the opening of the penis. Pain
and swelling in the testicles are uncommon.
Men or women who have receptive anal intercourse may acquire
chlamydial infection in the rectum, which can cause rectal
pain, discharge, or bleeding. Chlamydia can also be found
in the throats of women and men having oral sex with an infected
partner.
If untreated, chlamydial infections can progress to serious
reproductive and other health problems with both short-term
and long-term consequences. Like the disease itself, the damage
that chlamydia causes is often "silent".
Untreated infection can spread into the uterus or fallopian
tubes and cause pelvic inflammatory disease. Chlamydia can
also cause fallopian tube infection without any symptoms but
can lead to chronic pelvic pain and infertility.
 Complications
among men are rare. Infection sometimes spreads to the epididymis
(the tube that carries sperm from the testis), causing pain,
fever, and, very rarely, sterility. Complications
among men are rare. Infection sometimes spreads to the epididymis
(the tube that carries sperm from the testis), causing pain,
fever, and, very rarely, sterility.
Babies who are born to infected mothers can get chlamydial
infections in their eyes and respiratory tracts.
Chlamydia can be easily treated and cured with antibiotics.
A single dose of azithromycin or a course of doxycycline are
the most commonly used treatments.
All sex partners should be evaluated, tested, and treated.
Persons with chlamydia should abstain from sexual intercourse
for 7 days after a course of antibiotics to prevent spreading
the infection to their partners.
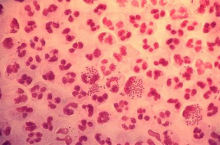 Gonorrhoea Gonorrhoea
Gonnorhoea is caused by a bacterium Neisseria gonorrhoeae,
that can grow and multiply easily in the warm, moist areas
of the reproductive system. It can also grow in the mouth,
throat, eyes, and anus.
Gonnorhoea is a very common infectious disease and is spread
through contact with the penis, vagina, mouth, or anus. Ejaculation
does not have to occur for gonnorhoea to be transmitted or
acquired. It can also be spread from mother to baby during
delivery.
 Any
sexually active person can be infected with gonnorhoea. People
who have had gonnorhoea and received treatment may get it
again if they have sexual contact with an infected person. Any
sexually active person can be infected with gonnorhoea. People
who have had gonnorhoea and received treatment may get it
again if they have sexual contact with an infected person.
Some men with gonnorhoea may have no symptoms at all. However,
most have signs or symptoms that appear one to fourteen days
after infection. Symptoms and signs include a burning sensation
when urinating, or a white, yellow, or green discharge from
the penis. Sometimes men with gonnorhoea get painful or swollen
testicles.
 In
women, the symptoms of gonnorhoea are often mild, but most
women who are infected have no symptoms. Even when a woman
has symptoms, they can be so non-specific as to be mistaken
for a bladder or vaginal infection. The initial symptoms and
signs in women include a painful or burning sensation when
urinating, increased vaginal discharge, or vaginal bleeding
between periods. Women with gonnorhoea are at risk of developing
serious complications from the infection, regardless of the
presence or severity of symptoms. In
women, the symptoms of gonnorhoea are often mild, but most
women who are infected have no symptoms. Even when a woman
has symptoms, they can be so non-specific as to be mistaken
for a bladder or vaginal infection. The initial symptoms and
signs in women include a painful or burning sensation when
urinating, increased vaginal discharge, or vaginal bleeding
between periods. Women with gonnorhoea are at risk of developing
serious complications from the infection, regardless of the
presence or severity of symptoms.
Symptoms of rectal infection in both men and women may include
discharge, anal itching, soreness, bleeding, or painful bowel
movements. Rectal infection also may cause no symptoms. Infections
in the throat may cause a sore throat, but usually causes
no symptoms.
Antibiotics can successfully cure gonnorhoea in adolescents
and adults. However, drug-resistant strains of gonnorhoea
are increasing in many areas of the world and successful treatment
of gonnorhoea is becoming more difficult.
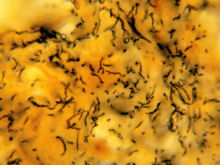
Syphilis
Syphilis is a sexually transmitted disease (STD) caused by
the bacterium Treponema pallidum. It has often been called
"the great imitator" because so many of the signs
and symptoms are indistinguishable from those of other diseases.
 Syphilis
is passed from person to person through direct contact with
a syphilis sore. Sores occur mainly on the external genitals,
vagina, anus, or in the rectum. Sores also can occur on the
lips and in the mouth. Transmission of the organism occurs
during vaginal, anal, or oral sex. Syphilis
is passed from person to person through direct contact with
a syphilis sore. Sores occur mainly on the external genitals,
vagina, anus, or in the rectum. Sores also can occur on the
lips and in the mouth. Transmission of the organism occurs
during vaginal, anal, or oral sex.
Pregnant women with the disease can pass it to the babies
they are carrying. Syphilis cannot be spread through contact
with toilet seats, doorknobs, swimming pools, hot tubs, bathtubs,
shared clothing, or eating utensils.
Many people
infected with syphilis do not have any symptoms for years,
yet remain at risk for late complications if they are not
treated.
Although transmission occurs from persons with sores who are
in the primary or secondary stage, many of these sores are
unrecognized. Thus, transmission may occur from persons who
are unaware of their infection.
 The
signs and symptoms of syphilis vary depending in which of
the four stages it presents (primary, secondary, latent, and
tertiary). The
signs and symptoms of syphilis vary depending in which of
the four stages it presents (primary, secondary, latent, and
tertiary).
The primary stage classically presents with a single chancre
(a firm, painless, non-itchy skin ulceration), secondary syphilis
with a diffuse rash which frequently involves the palms of
the hands and soles of the feet, latent syphilis with little
to no symptoms, and tertiary syphilis with neurological, or
cardiac symptoms.
Syphilis is believed to have infected 12 million people worldwide
in 1999, with greater than 90 percent of cases in the developing
world.
Syphilis is easy to cure in its early stages. A single intramuscular
injection of penicillin, an antibiotic, will cure a person
who has had syphilis for less than a year. Additional doses
are needed to treat someone who has had syphilis for longer
than a year. For people who are allergic to penicillin, other
antibiotics are available to treat syphilis. There are no
home remedies or over-the-counter drugs that will cure syphilis.
Treatment will kill the syphilis bacterium and prevent further
damage, but it will not repair damage already done.
 Blood
Borne Infections Blood
Borne Infections
HIV/AIDS
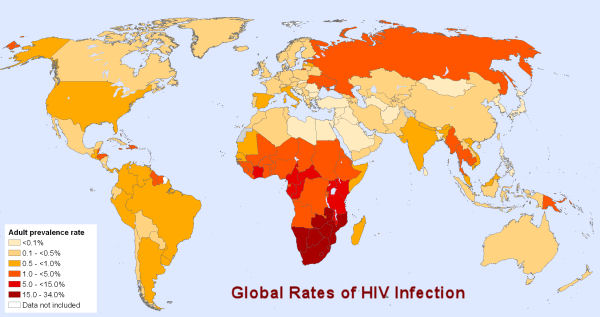
It is difficult to be sure about the risk of HIV infection
in different parts of the world. However, it is clear that
the infection is widespread and although the risk is high
amongst homosexual and intravenous drug using groups, on a
global scale, it is primarily a heterosexually spread disease.
Large numbers of the population in many parts of Africa are
infected and AIDS is common. Infection is also widespread
in other countries in Asia and South America. High proportions
of prostitutes are infected.
The
greatest increase in the number of HIV cases in the UK are
heterosexually acquired and about 75% of this figure can be
attributed to sex with a partner abroad.
 Human
immunodeficiency virus (HIV) is a member of the retrovirus
family that causes acquired immunodeficiency syndrome (AIDS),
a condition in humans in which progressive failure of the
immune system allows life-threatening opportunistic infections
and cancers to thrive. Infection with HIV occurs by the transfer
of blood, semen, vaginal fluid, pre-ejaculate, or breast milk. Human
immunodeficiency virus (HIV) is a member of the retrovirus
family that causes acquired immunodeficiency syndrome (AIDS),
a condition in humans in which progressive failure of the
immune system allows life-threatening opportunistic infections
and cancers to thrive. Infection with HIV occurs by the transfer
of blood, semen, vaginal fluid, pre-ejaculate, or breast milk.
Within these bodily fluids, HIV is present as both free virus
particles and virus within infected immune cells. The four
major routes of transmission are unsafe sex, contaminated
needles, breast milk, and transmission from an infected mother
to her baby at birth. Screening of blood products for HIV
has largely eliminated transmission through blood transfusions
or infected blood products in the developed world.
From its
discovery in 1981 to 2006, AIDS killed more than 25 million
people. HIV infects about 0.6% of the world's population and
in 2009 AIDS claimed an estimated 1.8 million lives including
approximately 260,000 children.
 A
disproportionate number of AIDS deaths occur in Sub-Saharan
Africa, retarding economic growth and exacerbating the burden
of poverty. A
disproportionate number of AIDS deaths occur in Sub-Saharan
Africa, retarding economic growth and exacerbating the burden
of poverty.
The only way to know whether you are infected is to be tested
for HIV. You cannot rely on symptoms alone because many people
who are infected with HIV do not have symptoms for many years.
Someone can look and feel healthy but can still be infected.
In fact, one quarter of the HIV-infected persons in the United
States do not know that they are infected.
Treatment with antiretroviral drugs reduces both the mortality
and the morbidity of HIV infection but antiretroviral medication
is still not universally available.
 HIV
infects vital cells in the human immune system such as helper
T cells and when these cell numbers decline below a critical
level, cell-mediated immunity is lost, and the body becomes
progressively more susceptible to opportunistic infections. HIV
infects vital cells in the human immune system such as helper
T cells and when these cell numbers decline below a critical
level, cell-mediated immunity is lost, and the body becomes
progressively more susceptible to opportunistic infections.
Most untreated
people infected with HIV eventually develop AIDS. These individuals
mostly die from opportunistic infections or malignancies associated
with the progressive failure of the immune system. HIV progresses
to AIDS at a variable rate but most will progress to AIDS
within 10 years of HIV infection.
Treatment
with anti-retrovirals increases the life expectancy of people
infected with HIV. Even after HIV has progressed to diagnosable
AIDS, the average survival time with antiretroviral therapy
was estimated to be more than 5 years.
Without antiretroviral therapy, someone who has AIDS typically
dies within a year.
 Viral
Hepatitis Viral
Hepatitis
"Hepatitis means inflammation of the liver and also refers
to a group of viral infections that affect the liver . The
most common types are Hepatitis A, Hepatitis B, and Hepatitis
C.
Viral hepatitis is the leading cause of liver cancer and the
most common reason for liver transplantation.
Hepatitis A
is a contagious liver disease that results from infection
with the Hepatitis A virus. It can range in severity from
a mild illness lasting a few weeks to a severe illness lasting
several months. Hepatitis A is usually spread when a person
ingests fecal matter — even in microscopic amounts —
from contact with objects, food, or drinks contaminated by
the feces or stool of an infected person.
The best way to prevent Hepatitis A is by getting vaccinated.
Hepatitis B
is a contagious liver disease that results from infection
with the Hepatitis B virus. It can range in severity from
a mild illness lasting a few weeks to a serious, lifelong
illness. Hepatitis B is usually spread when blood, semen,
or another body fluid from a person infected with the Hepatitis
B virus enters the body of someone who is not infected.
 This
can happen through sexual contact with an infected person
or sharing needles, syringes, or other drug-injection equipment.
Hepatitis B can also be passed from an infected mother to
her baby at birth. This
can happen through sexual contact with an infected person
or sharing needles, syringes, or other drug-injection equipment.
Hepatitis B can also be passed from an infected mother to
her baby at birth.
Hepatitis B can be either acute or chronic. Acute Hepatitis
B virus infection is a short-term illness that occurs within
the first 6 months after someone is exposed to the Hepatitis
B virus. Acute infection can — but does not always —
lead to chronic infection. Chronic Hepatitis B virus infection
is a long-term illness that occurs when the Hepatitis B virus
remains in a person’s body.
Chronic Hepatitis B is a serious disease that can result in
long-term health problems, and even death.
The best way to prevent Hepatitis B is by getting vaccinated.
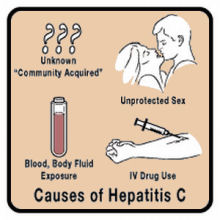 Hepatitis
C Hepatitis
C
is a contagious liver disease that results from infection
with the Hepatitis C virus. It can range in severity from
a mild illness lasting a few weeks to a serious, lifelong
illness. Hepatitis C is usually spread when blood from a person
infected with the Hepatitis C virus enters the body of someone
who is not infected. Today, most people become infected with
the Hepatitis C virus by sharing needles or other equipment
to inject drugs. Before 1992, when widespread screening of
the blood supply began in the United States, Hepatitis C was
also commonly spread through blood transfusions and organ
transplants.
Hepatitis C can be either “acute” or “chronic.”
Acute Hepatitis C virus infection is a short-term illness
that occurs within the first 6 months after someone is exposed
to the Hepatitis C virus. For most people, acute infection
leads to chronic infection. Chronic Hepatitis C is a serious
disease than can result in long-term health problems, or even
death.
There is no vaccine for Hepatitis C. The best way to prevent
Hepatitis C is by avoiding behaviors that can spread the disease,
especially injection drug use.
 Intravenous
Drug Abuse Intravenous
Drug Abuse
Drug-taking, apart from being illegal, might also put
the traveller in contact with people who are HIV positive
and should be avoided. Needle sharing is very dangerous.
Sharing needles to inject drugs or steroids is another way
that HIV can be passed to other people. Sharing of needles
for tattoos, piercings, and body art can also lead to infection.
Someone with HIV who shares a needle also shares the virus,
which lives in the tiny amounts of blood attached to the needle.
Sharing needles also can pass hepatitis and other serious
infections to another person.
| Beware:
Draconian Drug Laws |
|
 Southeast
Asia’s governments impose the toughest drug laws
on the planet. You can’t blame them – the
legendary “Golden Triangle”, an area bordering
Thailand, Laos and Myanmar, is right in the heart of
the region, and is a world hotspot of narcotics production. Southeast
Asia’s governments impose the toughest drug laws
on the planet. You can’t blame them – the
legendary “Golden Triangle”, an area bordering
Thailand, Laos and Myanmar, is right in the heart of
the region, and is a world hotspot of narcotics production.
Many other countries impose harsh penalties for the
posesssion and/or trafficking of illegal drugs. Very
long prison sentences and even the death sentence have
been handed out to travellers carrying illicit substances;
so don't be tempted!
In spite of such draconian measures, certain places
are flush with illegal drugs. However, you should still
defer to local laws if offered a chance to indulge –
your status as a foreigner does not make you less likely
to be punished for drug use, quite the opposite!
Some general advice:
-
Don’t bring illegal drugs with you. Don’t
get conned into carrying drugs for others, whether
as personal favors or for profit. The risks far outweigh
the possibility of getting away with it.
- If
you’re bringing prescription drugs with you,
play it safe and bring the prescription for these
drugs.
|
|
 An
alarming research study recently published discovered
that the "innocent" commercial tattoo may
be the number one distributor of hepatitis C. An
alarming research study recently published discovered
that the "innocent" commercial tattoo may
be the number one distributor of hepatitis C.
The
study found that commercially acquired tattoos accounted
for more than twice as many hepatitis C infections as
injection-drug use. This means it may have been the
largest single cause of this form of hepatitis and you
are twice as likely to be infected with hepatitis C
from getting a tattoo from a tattoo shop than shooting
up drugs.
The
study focussed on "sanitized" commercial tattoo
parlours and not so called back-street or prison tattoos.
When
you consider hepatitis B can be transmitted with as
little as 0.00004 ml of blood, and can live on blood
contaminated surfaces, such as needles, tattoo machines,
tables, etc. for over two months, the risk of hepatitis
is very real indeed.
|
Tattoos,
piercing and HIV / Aids infection
Australian health officials are urging travellers to avoid
getting tattoos in developing countries after it was reported
a West Australian man contracted HIV after getting etched
in Bali.
When you think of having a tattoo done, first of all remember
that it involves your skin being pierced and forming an open
sore, and that blood will also be involved in this procedure.
 Although
body art and tattoos are very popular some safety measures
must be taken. Since piercing the skin, and blood and needles
are involved some warning lights should be going off, since
working with open "wounds" and blood opens the entire
Pandora's box of Aids and Hepatitis infection. Although
body art and tattoos are very popular some safety measures
must be taken. Since piercing the skin, and blood and needles
are involved some warning lights should be going off, since
working with open "wounds" and blood opens the entire
Pandora's box of Aids and Hepatitis infection.
In saying this, the risk of HIV as well as hepatitis transmission
exists if ANY of the instruments are not properly sterilized
and disinfected. When having a tattoo, ask the person doing
it what type of safety precautions are taken to prevent the
spread of blood borne infections, such as HIV or hepatitis.
Unless you are absolutely certain that the equipment being
used is sterile, skin-damaging procedures such as ear piercing,
tattooing and acupuncture should be avoided.
Health standards in many developing countries are drastically
different to those in more developed nations, and this should
be kept in mind at all times.
 Hepatitis
C is spread by infected blood and infected needles, which
is the virus' connection with tattooing. Tattoos involve lots
of needles making lots of sticks in the skin. Each stick carries
potential for contamination -- and not just with hepatitis,
but also HIV. Hepatitis
C is spread by infected blood and infected needles, which
is the virus' connection with tattooing. Tattoos involve lots
of needles making lots of sticks in the skin. Each stick carries
potential for contamination -- and not just with hepatitis,
but also HIV.
The prospect of a cheap tattoo might sound good for the wallet,
but the risks associated with it are just too high - it's
just not worth it.
Aside from the health risks, some tattoos from developing
nations use cheap inks, which can run and blotch after a short
time - it's best to avoid it all together, and wait until
you get to a parlour that offers certifiable health standards.
It is strongly recommended that people who have had tattoos
whilst travelling abroad get a Hepatitis check as soon as
possible. Hepatitis can lie unnoticed for many years while
doing serious damage. The sooner hepatitis is detected the
better the chances for survival. If you have a tattoo –
get checked.
| Some
pointers when selecting a tattoo artist or piercing operator |
-
New
sterile sealed needles must ALWAYS be used.
-
He/she
must use new needles at all times and the tattoo
artist must be disposing of used needles in a responsible
way after autoclaving them.
-
New
needles come in sterile sealed packages and INSIST
ON SEEING THE SEALED STERILE PACKAGE before the
body artist starts creating your body art tattoo.
-
The
working area must be neat and clean and must be
sterilized after each customer to minimize the risk
of any infection.
-
New
unused razors must be used when shaving hair from
areas to be tattooed.
-
A
new container of ink must be used for EACH CLIENT.
-
A
health board license must be clearly displayed (if
applicable) to attest that the premises and practice
have passed health standards.
-
Also
check your local city ordinances to see what safety
rules apply in your area.
|
 Medical
Care Medical
Care
In many
developing countries standards of infection control may be
inadequate to prevent the spread of blood borne infections.
Instruments may not be sterilised between patients and re-use
of medical supplies, including needles and syringes is common.
Travel packs are available from chemists and travel clinics,
containing sterile equipment for use in an emergency. These
kits should be supplied with a certificate showing contents
and the reason for its purchase, useful for customs clearance.
Blood
transfusion: In most of Western Europe, North America,
Japan and Australasia all donated blood is now screened for
HIV antibodies.
However, in many developing countries there may be
only the most basic blood transfusion services and much of
the blood donated is unscreened. The risks from blood transfusion
in such circumstances are high. Thus, points to consider are:
|
-
Accidents
are the commonest reason for needing a blood transfusion
so they should be avoided where possible by taking
extra care and vigilance, e.g. driving carefully
in foreign countries.
-
Blood
transfusion should only be accepted when essential.
-
Pregnancy
or any medical condition which may lead to heavy
blood loss, should be taken into account before
travelling to destinations where good medical facilities
will not be available.
-
Knowing
your blood group in advance may make it easier to
find a blood donor in an emergency.
|
 Hepatitis
B Vaccine Hepatitis
B Vaccine
Hepatitis
B is a serious illness which is spread as described above.
Symptoms include chronic fatigue, loss of appetite, fever
and jaundice. In a small percentage of individuals the disease
may cause permanent damage or liver cancer.
 Fortunately
there is a vaccine available which gives good protection against
the disease. However, it can take up to six months to become
effective. Fortunately
there is a vaccine available which gives good protection against
the disease. However, it can take up to six months to become
effective.
Vaccination
is recommended for those travelling to areas of high prevalence
who plan to remain there for lengthy periods such as voluntary
workers, who may be at risk from medical or dental procedures
carried out in those countries.
Short
term travellers are not generally at risk but may place
themselves at risk by their sexual behaviour. It is given
as a course of three 1ml intra-muscular injections, the second
28 days after the first and the third 6 months after the second.
|